Orthopedics
Healing Bones, Joints & Muscles
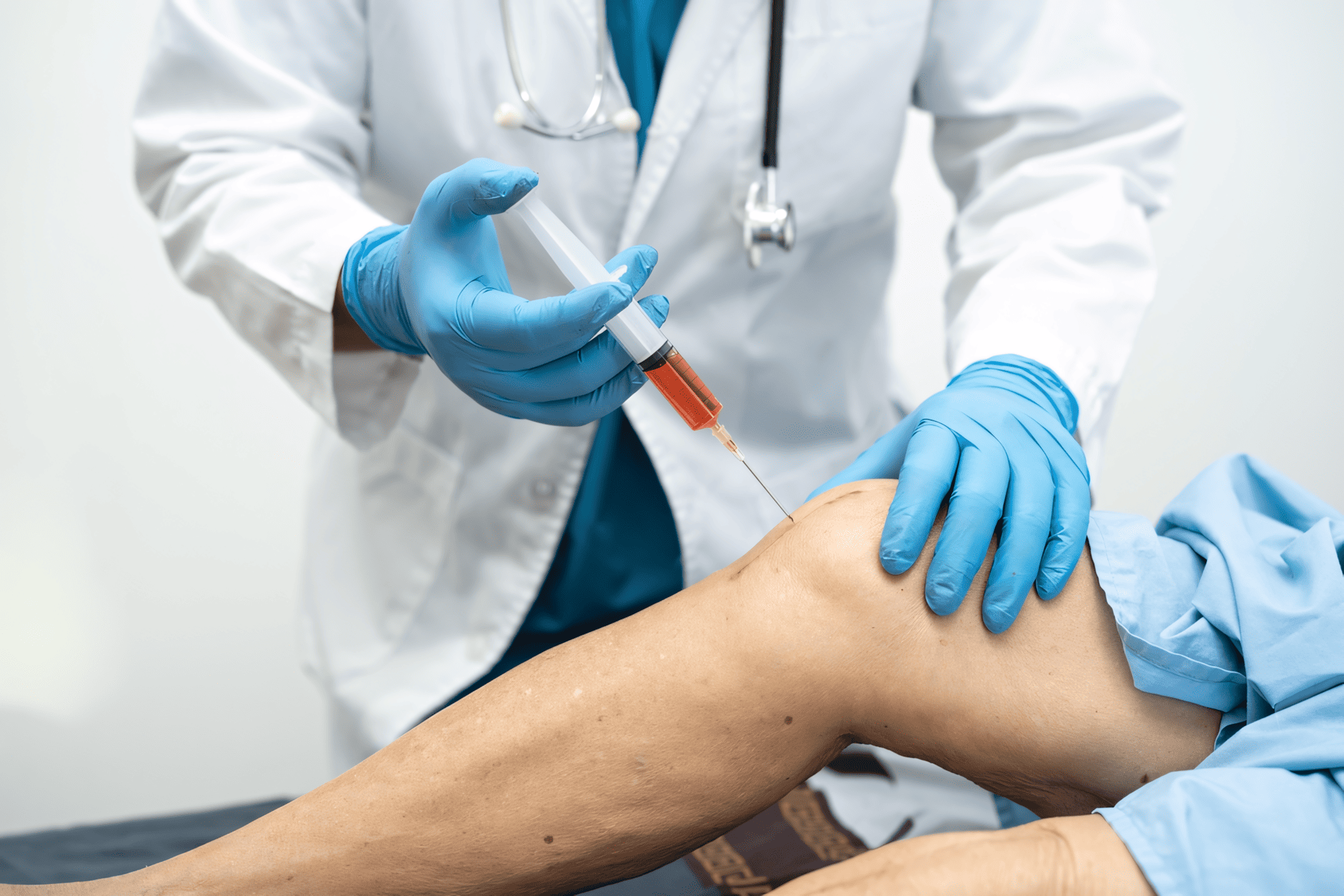
Welcome to Rejuvenate
Regenerative Medicine: A Revolutionary Approach to Healing
At Plus91 Aesthetics, we believe in harnessing the body’s natural ability to heal through Regenerative Medicine—a cutting-edge approach utilizing cell therapy, tissue engineering, and biologics to repair and regenerate damaged tissues.
Unlike conventional treatments that merely manage symptoms, regenerative medicine addresses the root cause of orthopedic conditions, promoting natural healing and recovery.
These non-surgical, painless procedures, performed on an OPD basis, serve as excellent alternatives to NSAIDs, steroids, and even surgeries.
Advanced Regenerative Orthopedic Treatments
Joint Care
1. PRP Injection (Recommended)
- Ideal for Stage 1 and Stage 2 arthritis
- Helps reduce pain, inflammation, and degeneration
2. PRP Hyaluronic Injection
- Recommended for patients between Stage 2 and 3 arthritis
- Enhances joint lubrication, promoting smoother movement and delaying degeneration
3. PRP for Cartilage Implantation (Micrografting)
- Recommended for Stage 3 or more arthritis
- Also known as micrografting, helps regenerate damaged cartilage
Soft Tissue & Tendon Care
- PRP Therapy for tendon injuries, including rotator cuff tears, tennis elbow, and Achilles tendinopathy
- Regenera Activa AMT (Autologous Micrograft Technology) for enhanced soft tissue healing and cellular
repair - Stem cell therapy for ligament and tendon regeneration
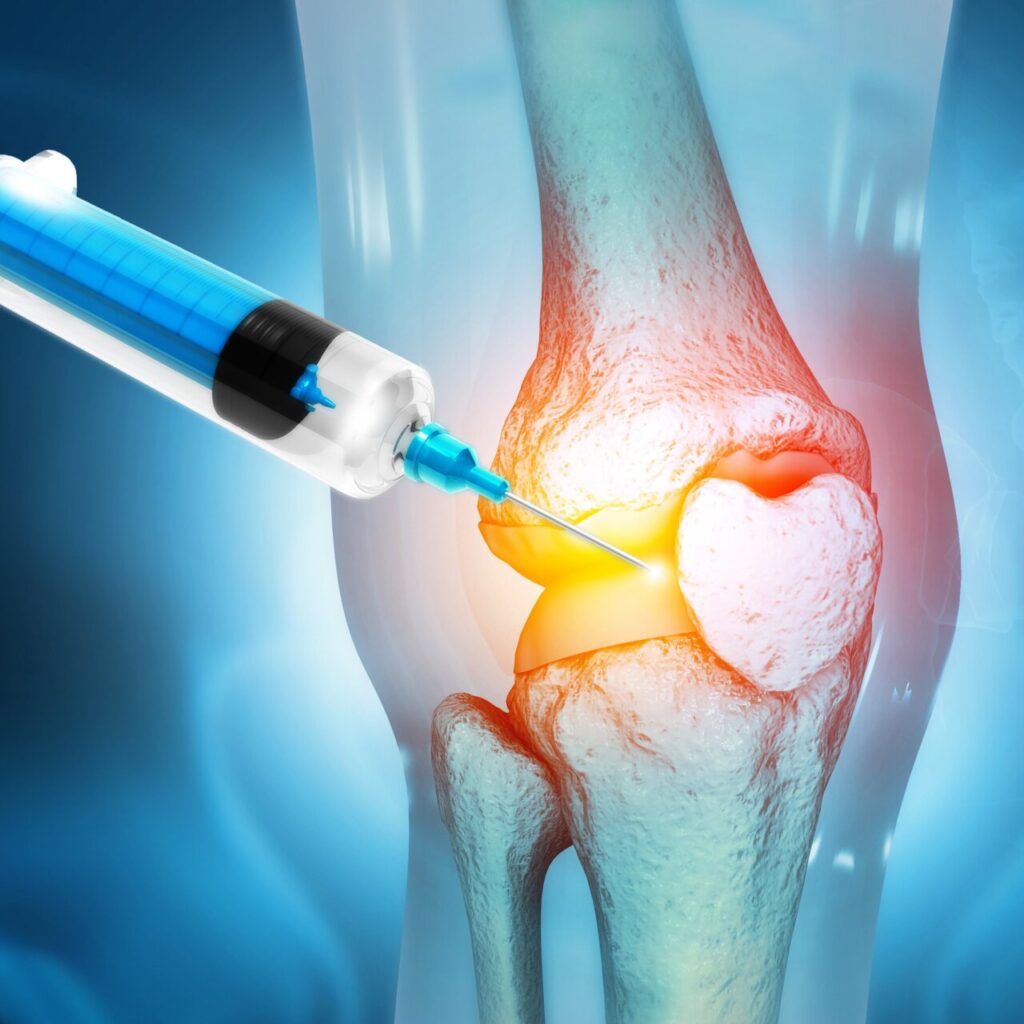
Platelet Rich Plasma for Knee Osteoarthritis: When it works, when it does not work
Part 1: An introduction to PRP treatments.
The science PRP as an anti-inflammatory. Chronic inflammation from structural breakdown caused by knee instability. Platelet-rich plasma can provide key factors balancing proinflammatory and anti-inflammatory factors. PRP as an anti-inflammatory. Chronic inflammation from structural breakdown caused by knee instability.
Platelet-rich plasma can provide key factors balancing proinflammatory and anti-inflammatory factors. Runaway, chronic inflammation destroys the extracellular matrix (ECM) in the osteoarthritic knee. Stopping extracellular matrix dilution is one of the healing factors in PRP.
One of the characteristics of PRP is that it works to change the chemical milieu of the joint environment. It sent the chemical signals necessary to strategically shut down this inflammation harmful to the extracellular matrix.
Part 2: Do Platelet-rich plasma injections delay the need for knee replacement?
- Does PRP really work in helping people avoid knee replacement?
- “Platelet-rich plasma injections delay the need for knee replacement” – “85.7% of the patients did not undergo total knee replacement during the five-year follow-up.”
- PRP research into cartilage repair.
- MRI evidence that PRP regrows cartilage in knee patients.
- Research with no cartilage growth. PRP and Stage IV osteoarthritis.
Part 3: When PRP works – patient outcome research
- The evidence for PRP knee osteoarthritis treatments as an effective treatment.
- That said, earlier research suggests that PRP injection does result in improved knee pain and function in patients with osteoarthritis.
- Overall, 60% of patients from stage 2 to stage 4 osteoarthritis had good outcomes with PRP and less knee pain.
- Another study suggests a 70% improvement in knee pain after PRP treatments in Garde 1 to Grade 3 patients.
- In one paper – long-term meaningful results were seen in 85% of patients in knee pain after PRP treatments.
- Women show a positive response to platelet-rich plasma despite presenting more painful knee osteoarthritis than men.
Part 4: Comparisons between PRP and Hyaluronic Acid
- “Patients undergoing treatment for knee osteoarthritis with PRP can be expected to experience improved clinical outcomes when compared with hyaluronic acid.”
- A simple comparison of treatments between PRP, NSAIDs, hyaluronic acid, and placebo.
- PRP as knee lubricant substance.
- PRP and hyaluronic acid injections used together.
- Hyaluronic acid injections with combined PRP treatment versus using hyaluronic acid injections alone in knee pain patients.
Part 5: PRP, Cortisone, Hyaluronic Acid, Ozone Therapy
- Two groups of patients, one group gets PRP for knee pain the other group gets cortisone for knee pain. How did this comparison work out?
- Cortisone is a one-shot treatment, PRP should not be given the same way. This is when PRP does not work for knee pain.
- The difference in the side-effects. PRP has little risk of side effects, cortisone greater chance of side effects.
- Cortisone is manly a one-shot treatment, PRP should not be given the same way. This is when PRP does not work for knee pain.
- Comparisons of PRP, Cortisone and Hyaluronic Acid.
- Comparison of PRP and Ozone Therapy.
- One injection of bone marrow aspirate concentrate stem cells versus one injection of PRP.
- PRP or TENS treatment for knee pain?
Regenera ATM (Autologous Tissue Micrografting)
Regenera ATM (Autologous Tissue Micrografting)
Regenera ATM is a minimally invasive, regenerative medicine treatment for knee pain caused by conditions like osteoarthritis, cartilage damage, or joint degeneration. It uses the patient’s own tissue to promote healing and reduce inflammation.
How Does Regenera ATM Work?
1. Tissue Extraction – A small sample of tissue (usually from behind the ear or abdomen) is taken.
2. Micrografting – The tissue is processed to extract regenerative cells, growth factors, and anti-inflammatory proteins.
3. Injection – The concentrated solution is injected into the affected knee joint* to stimulate repair.
Benefits for Knee Pain
✔ Reduces inflammation & pain
✔ Promotes cartilage regeneration
✔ Minimally invasive (no surgery)
✔ Uses patient’s own cells (low risk of rejection)
✔ Short recovery time
Conditions Treated
– Osteoarthritis (OA) of the knee
– Cartilage wear & tear
– Chronic joint pain
– Post-injury knee degeneration
Effectiveness & Recovery
– Some patients report pain relief within weeks.
– Full effects may take 2-3 months as tissue regenerates.
– No major downtime (unlike knee replacement).
Comparison to Other Treatments
| Treatment | Invasiveness | Recovery Time | Longevity |
| Regenera ATM | Minimally invasive | Days to weeks | Months to years |
| PRP Therapy | Injection-based | 1-2 weeks | 6-12 months |
| Stem Cell Therapy | Moderate | Weeks | 1+ years |
| Knee Replacement | Major surgery | 3-6 months | 10-15 years |
Who Is a Good Candidate?
– Patients with *mild to moderate knee arthritis
– Those looking for non-surgical options
– People who haven’t responded well to steroids or PRP
Limitations
❌ Not for severe arthritis (bone-on-bone cases may need surgery)
❌ Cost may be high (varies by clinic)
❌ Not universally available
Would you like help finding clinics that offer Regenera ATM for knee pain* in India?
Why Choose Regenerative Orthopedic Treatments?
Minimally invasive & painless procedures performed in an outpatient setting
Faster recovery time with no hospital stay required
Avoidance of steroids and NSAIDs, reducing long-term side effects
Enhanced mobility, strength, and pain relief with long-lasting effects
Schedule a consultation today!
At Plus91 Aesthetics, under the expertise of Dr. Aleem A. Siddiqui, we bring world-class Regenerative Medicine solutions to improve mobility, alleviate pain, and restore quality of life.
Schedule a consultation today and take the first step towards natural healing and long-term recovery.
What are the different types of orthobiologics?
Biologics are isolated (taken from) from a variety of natural sources — human, animal, or micro-organism. Biologics can be:
Composed of sugars, proteins, or nucleic acids, or complex combinations of these substances
Living entities, such as cells and tissues
Some examples of biologics used in orthopaedics include:
Stem cell treatments (as part of an FDA-approved trial)
Blood products, such as platelet-rich plasma (PRP)
Viscosupplementation products used to treat arthritis
How are biologics currently being used in orthopaedic care — for which conditions and injuries?
Because orthobiologics are still relatively new, the evidence supporting their use is limited. That said, biologic therapies have shown promise when used:
To treat tendinopathies, such as tennis elbow (lateral epicondylitis)
To treat pain from early arthritis, including early knee osteoarthritis, which can help delay the need for surgery
As an aid to healing after surgery to repair certain tendons, including rotator cuff repair
To treat avascular necrosis (death of bone tissue resulting from temporary or permanent loss of blood supply to the bone)
ow are biologics thought to work and improve symptoms?
What does scientific evidence say about the effectiveness of orthobiologic therapies?
Who could potentially benefit from orthobiologic treatments?
There is potential for benefit from orthobiologics in many areas of orthopedics to treat numerous common conditions.
Are orthobiologics safe? What are the potential risks?
Generally speaking, biologic materials harvested (taken) from your own body and used to treat you the same day have been felt to be safe enough to permit their use without extensive FDA approvals. There can still be risks, however, and you should discuss these risks with your doctor.
According to the Food and Drug Administration (FDA), “… Unproven stem cell therapies can be particularly unsafe.” (See full article here). Because stems cells do not come from your own body, and are further manipulated in a laboratory, these treatments pose additional risks and can be offered only in an FDA-approved clinical trial. Ask your doctor if the stem cell treatment they offer is part of an FDA-approved trial.
With so many places offering biologic therapies, how do I know which doctors I can trust?
While trustworthy doctors can be found in many areas, if your doctor is board certified and a fellow of the American Academy of Orthopedic Surgeons (FAAOS), it means they have met the rigorous professional and ethical standards established by AAOS — the trusted leader in musculoskeletal health.
Do orthobiologic therapies involve fetal stem cells?
Generally speaking, biologic materials harvested (taken) from your own body and used to treat you the same day have been felt to be safe enough to permit their use without extensive FDA approvals. There can still be risks, however, and you should discuss these risks with your doctor.
According to the Food and Drug Administration (FDA), “… Unproven stem cell therapies can be particularly unsafe.” (See full article here). Because stems cells do not come from your own body, and are further manipulated in a laboratory, these treatments pose additional risks and can be offered only in an FDA-approved clinical trial. Ask your doctor if the stem cell treatment they offer is part of an FDA-approved trial.
Does insurance, including Medicare, cover orthobiologic treatments?
Many orthobiologic treatments, even those approved by the FDA, may not be covered by your insurance.
Be sure to ask your insurance provider about whether a specific biologic treatment is covered for your specific condition before starting the treatment.
How much do orthobiologic therapies typically cost?
Costs vary for each type of biologic and for each doctor or facility. These costs need to be reviewed with your doctor.
Be a savvy consumer; carefully weigh the cost of the treatment against the available information on its effectiveness, as well as the risks and benefits, before starting.

Dr. Aleem A. Siddiqui
(MBBS, MS (Orthopaedics))
Orthopedic Specialist
Dr. Aleem A. Siddiqui is a highly skilled orthopedic specialist with extensive training from leading medical institutions across the UK, Germany, Austria, Portugal, Estonia, Singapore, Bangkok, and Bulgaria.
His expertise spans joint replacement, trauma, and spine surgeries, and he has received a fellowship from the American Academy of Orthopedic Surgery (Garcia De Orta Hospital, Almada, Lisbon, Portugal).
Having served in esteemed institutions like Robert Jones and Agnes Hunt Orthopaedic Hospital (UK) and Royal Glamorgan Hospital (Wales), Dr. Siddiqui brings unparalleled expertise in regenerative medicine
- Location: Byculla East, Mumbai
- Experience: 24+ Years
- Clinics: Plus91 Aesthetics | M.H. Saboo Siddique Maternity & General Hospital
- For Appointment: +91 7208017070
- Email: draleemsiddiqui@gmail.com
- Visit Us: www.plus91aesthetics.com
